Jump to section
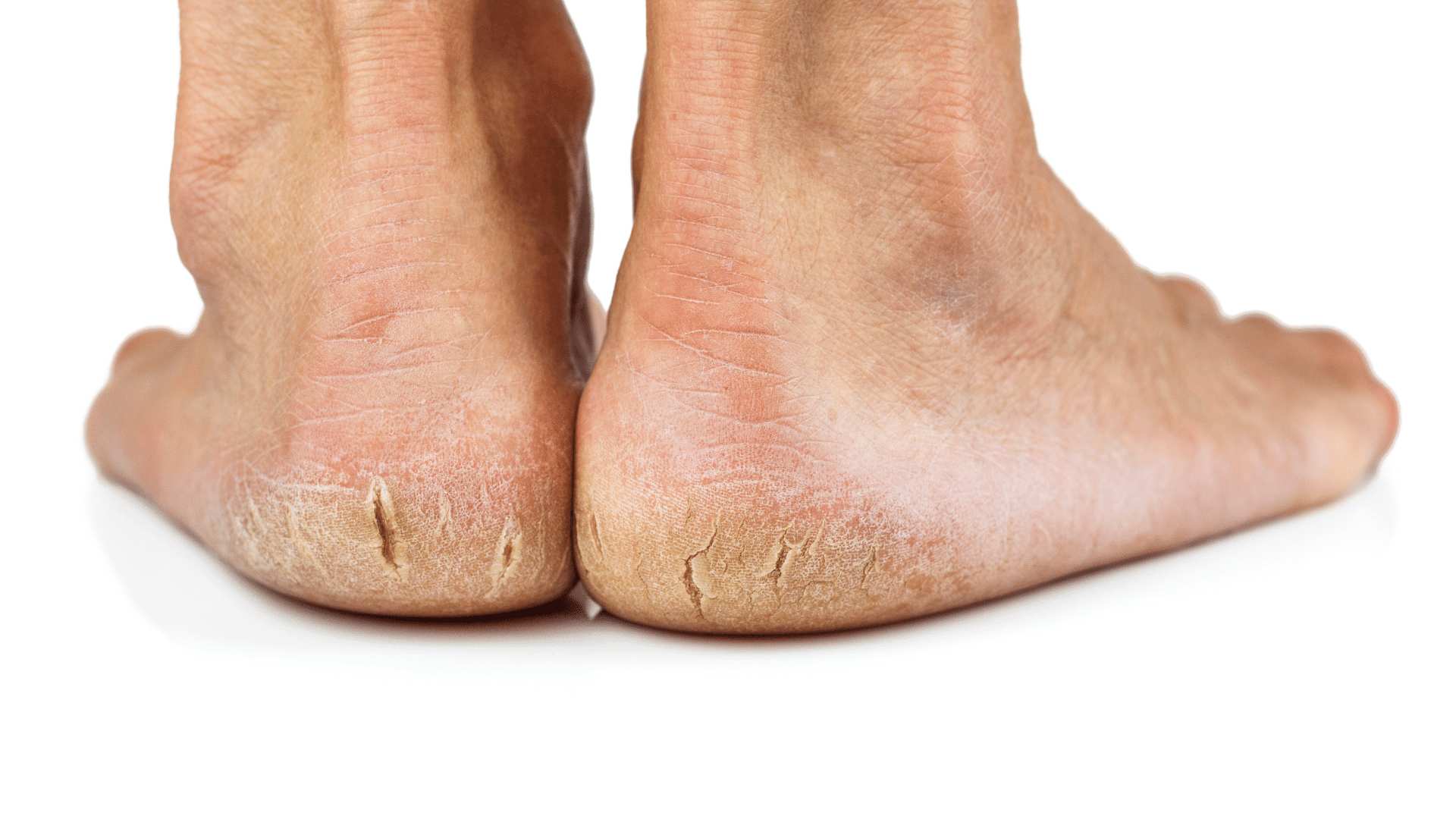
A cracked heel is a common foot problem. It occurs when dry, thick skin on the bottom of your heels cracks and splits.
In most cases, if the cracks are minor, it’s merely a nuisance and may be unattractive to look at, but if left untreated and the heel fissures become deeper, it can be painful to walk and may become infected.
There are several stages of developing a cracked heel. The first sign is the formation of dry, hard skin around the heel — these are called calluses. As you walk and put more pressure on the area, the fat pads under your heels expand, causing these calluses to start to develop small cracks.
Other factors that can cause cracked heels include:
Over time, the cracks will become deeper and they may begin to bleed. In severe cases, the cracks can lead to infection and if you are a diabetic, cracked heels can lead to diabetic foot ulcerations.
As well as the physical appearance of dry and cracked skin on your heels, you may also experience the following symptoms:
How do you usually treat dry skin? You moisturise!
If your condition is minor, start by moisturising your heels 2-3 times per day to help relieve your symptoms. You can use a pumice stone prior to moisturising, to remove any hard, dead skin that may prevent the moisturiser from sinking in effectively.
After a week of general foot care, if your symptoms persist, it may be time to consult one of our podiatrists. Our podiatrists in Brisbane may recommend or administer a combination of the following treatments:
We can also perform pressure assessments and utilise such technology to determine the amount of pressure your heel is experiencing when you walk. We can then reduce the pressure to avoid callus build up.
There are a number of approaches you can take to prevent yourself from getting cracked heels.

The more tense you (or your muscles, ligaments and all sorts of fibres) feel, then the more pain you will understandably perceive. Here are
three ways to help relieve this tension in your feet.

Not everyone needs orthotics, but they can play an integral role in treating or relieving pain in several foot and lower limb conditions.

The heat and humidity of an Australian summer makes it a prime time for issues to arise, so our newest podiatrist Lucy has put together
seven helpful tips to keep your feet healthy and problem free throughout summer.
| Monday | 7:40am - 6:00pm |
| Tuesday | 7:40am - 6:00pm |
| Wednesday | 7:40am - 6:00pm |
| Thursday |
7:40am - 6:00pm |
| Friday | CLOSED |
| Saturday | CLOSED |
| Sunday | CLOSED |
Ground Floor, 344 Queen Street,
Brisbane City QLD 4000
| Monday | 7:40am - 6:00pm |
| Tuesday | 7:40am - 6:00pm |
| Wednesday | 7:40am - 6:00pm |
| Thursday |
7:40am - 6:30pm |
| Friday | 7:40am - 5:00pm |
| Saturday | 7:40am - 4:30pm |
| Sunday | CLOSED |
Newmarket Village, 114/400 Newmarket Rd, Newmarket QLD 4051