Jump to section
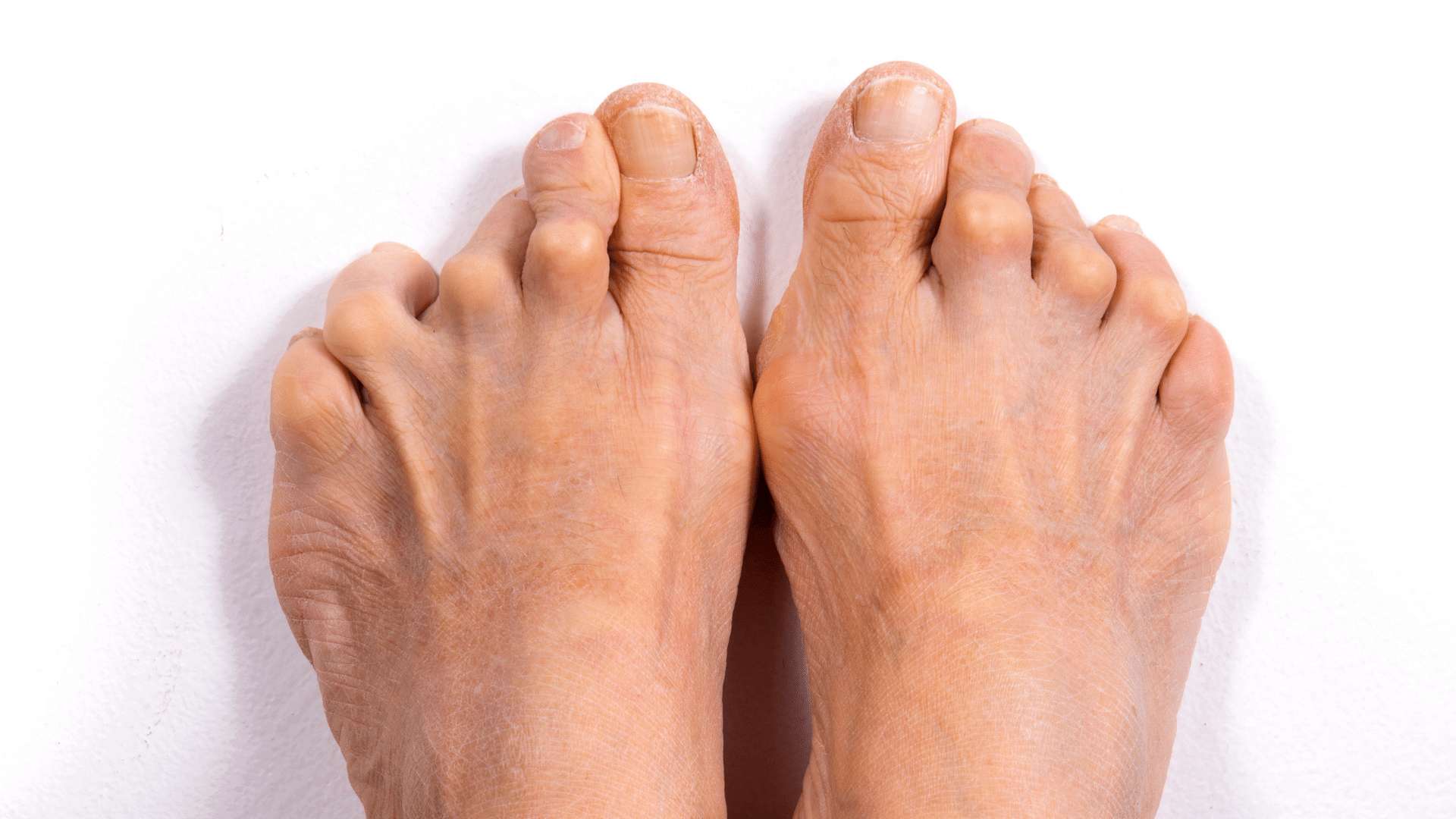
Living with rheumatoid arthritis can be taxing on a person’s mobility and quality of life, especially if they’re experiencing significant joint deformities and swelling in their feet. Our Brisbane podiatrists have a range of therapies and management strategies to best support those with rheumatoid arthritis and help optimise their mobility, so they can keep doing the things they love.
Rheumatoid arthritis is a long-term autoimmune condition that affects your body by persistently attacking the lining of your joints,
ultimately leading to their damage and deterioration. Unlike the wear-and-tear damage of osteoarthritis
that happens with use over time, this occurs when the immune system doesn't work properly, mistakenly attacking your own healthy
cells.
One of the distinguishing factors of rheumatoid arthritis is its symmetry, affecting the joints on both the left and right side of your body and across multiple joints. This is vastly different to osteoarthritis, which is commonly unilateral and isolated to minimal joints, or gout where only very few joints are affected - often only the big toe joint on one foot.
The joints commonly involved in rheumatoid arthritis include the small joints of your hands and feet, knees, hips, ankles, elbows and shoulders. In some people, the disease will affect more than just your joints, and may cause damage to your skin, eyes, lungs, heart and blood vessels.
For most people, your immune system serves to defend your body against infection. With rheumatoid arthritis, your immune system malfunctions
and mistakes your body's cells for invaders - attacking them instead. This results in the release of inflammatory chemicals that attack the synovium,
the soft tissue that lines the joints and produces a fluid that helps your joints move smoothly and without friction. When the synovium
becomes inflamed, it thickens, causing the area to feel painful and tender, become red and swollen, and it can even minimise movement around
the joints leading to stiffness and difficulty bearing weight on the joints.
Over time, this process eventually deteriorates the cartilage and bone within the affected joints. Additionally, the tendons and ligaments responsible for supporting and stabilising your joints will weaken and stretch, causing the joint to lose its shape and alignment - leading to deformed and disfigured joints that can make it difficult to walk or find well-fitting footwear.
It is not currently known why your immune system decides to attack your body instead of the intruders. Researchers believe it could be connected to your genetics paired with environmental or other triggers. This means that having certain genes, when activated by an environmental trigger, such as a virus or bacteria, may trigger the disease.
Factors that may increase your risk of developing rheumatoid arthritis, including:
Symptoms of rheumatoid arthritis can vary greatly from person to person, ranging from mild to severe. In the early days of the disease, you
may not see large amounts of swelling or redness, however, you are still likely to experience pain and tenderness. As the inflammation
continues and the joint damage accumulates, you may start to notice visible changes in the stiffness, structure and function of your joints.
General signs and symptoms include:
Rheumatoid arthritis will mostly affect the smaller joints first, particularly the joints that attach your fingers to your palms and toes to your feet. It may then spread to your larger joints including your knees, hips, ankles, elbows, shoulders and wrists. These symptoms will often appear as flare ups or exacerbations, when you're experiencing a lot of inflammation and other symptoms. These can last for days or months, and are usually followed by periods of apparent remission, when the swelling and pain seem to disappear.
Rheumatoid arthritis can be difficult to recognise and diagnose in its early stages as the early symptoms mimic those of many other
conditions and diseases. Due to this, and the fact that early interventions can help optimise your comfort and mobility over the years,
it’s important to get an accurate diagnosis early.
Diagnosing rheumatoid arthritis starts with getting a detailed look into your medical history and then completing a comprehensive physical examination of your symptoms; particularly looking for tender and warm joints, localised joint inflammation and pain during joint movement, bony alignment change and reduction in joint movement. If rheumatoid arthritis is suspected, the next step is a referral for blood tests that will look for inflammation and the presence of specific blood proteins. Your GP may also need to carry out additional testing, such as:
Our podiatrists may also request an x-ray, ultrasound or MRI to reveal any joint damage and the extent of it, as rheumatoid arthritis can
cause the ends of the bone to wear down. If no damage shows up in these first tests, that may confirm the disease is in an early stage that
hasn't damaged the bone yet. This is valuable information for your podiatrist to know in terms of developing a tailored management plan that
will best support your joints, feet and legs.
While there is currently no “cure” for rheumatoid arthritis, the symptoms can definitely be managed and reduced when detected early and treatment is started. Effectively managing rheumatoid arthritis means working with a multidisciplinary care team that may involve your doctor, rheumatologist, podiatrist and other health professionals. Many people diagnosed with rheumatoid arthritis will be prescribed medications such as non-steroidal anti-inflammatory drugs (NSAIDs), disease-modifying antirheumatic drugs (DMARDs), janus kinase inhibitors (JAKs) and corticosteroids. These can go a long way in helping reduce episodes of significant swelling, pain and discomfort.
Regardless of whether your rheumatoid arthritis is in its early stages or if notable joint damage has occurred, there is a lot that our podiatrists can do to help optimise your comfort on your feet, your mobility and your quality of life. Our Brisbane podiatrists work extensively with those with rheumatoid arthritis, using therapies and management strategies including:
If left untreated, rheumatoid arthritis can cause a number of complications including, but not limited to:
Although not knowingly preventable, there are a few things you can do to decrease your risk of developing rheumatoid arthritis:
Our feet are the foundation for the entire body, so it's important that they have enough strength to tolerate our activity levels. Use
these three exercises to help strengthen your feet.

Not everyone needs orthotics, but they can play an integral role in treating or relieving pain in several foot and lower limb conditions.

The heat and humidity of an Australian summer makes it a prime time for issues to arise, so our newest podiatrist Lucy has put together
seven helpful tips to keep your feet healthy and problem free throughout summer.
| Monday | 7:40am - 6:00pm |
| Tuesday | 7:40am - 6:00pm |
| Wednesday | 7:40am - 6:00pm |
| Thursday |
7:40am - 6:00pm |
| Friday | CLOSED |
| Saturday | CLOSED |
| Sunday | CLOSED |
Ground Floor, 344 Queen Street,
Brisbane City QLD 4000
| Monday | 7:40am - 6:00pm |
| Tuesday | 7:40am - 6:00pm |
| Wednesday | 7:40am - 6:00pm |
| Thursday |
7:40am - 6:30pm |
| Friday | 7:40am - 5:00pm |
| Saturday | 7:40am - 4:30pm |
| Sunday | CLOSED |
Newmarket Village, 114/400 Newmarket Rd, Newmarket QLD 4051