Jump to section
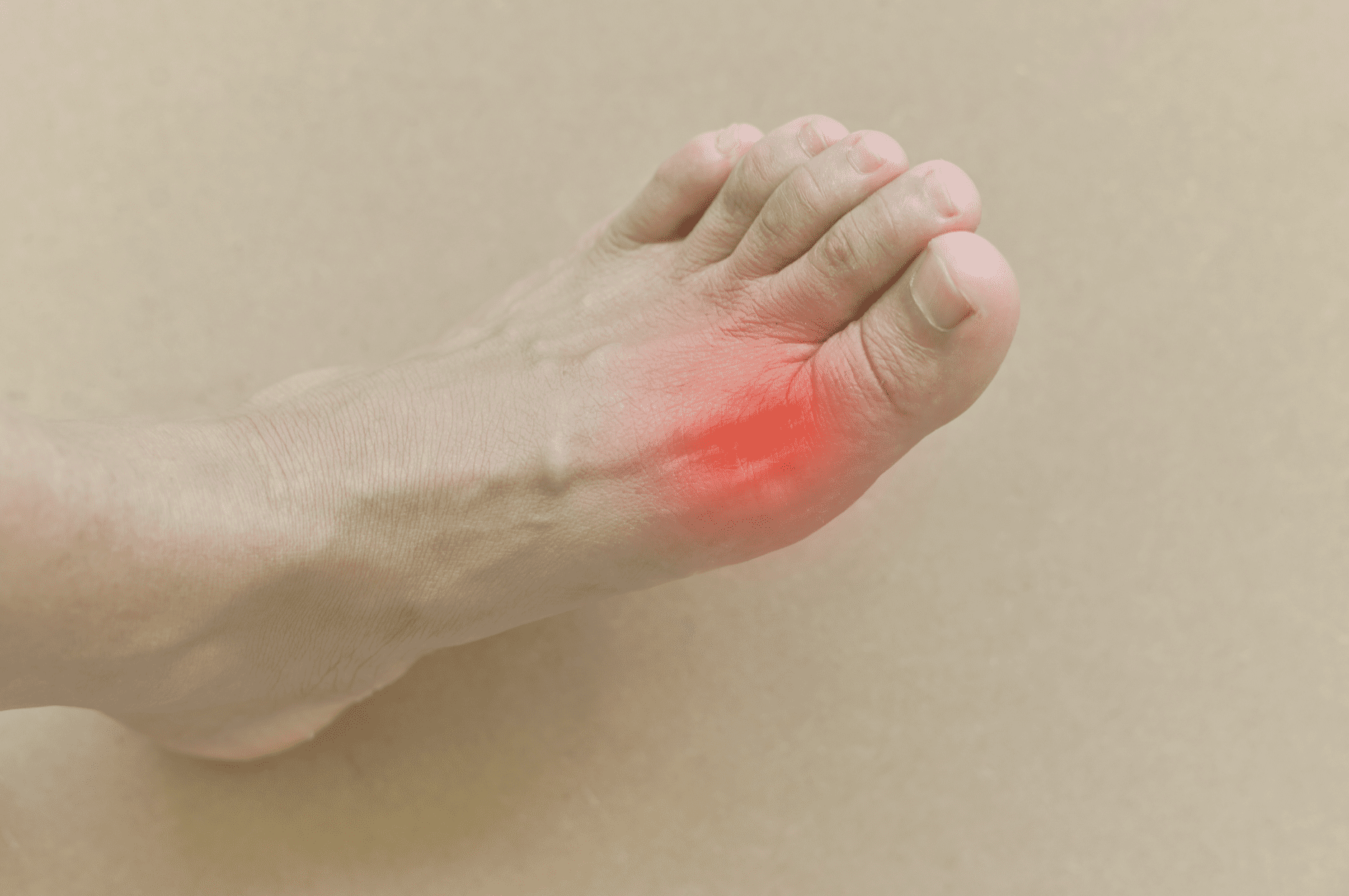
Gout is an inflammatory arthritis that most often affects the big toe joint. It occurs when uric acid builds up to a high concentration in
the blood, creating extremely painful crystal deposits in the affected joints.
Gout is a type of arthritis that is very different from its auto-immune or wear-and-tear counterparts. Instead of being linked to degeneration over time like in osteoarthritis, or being caused by your body attacking its own cells (typically in a symmetrical pattern) like in rheumatoid arthritis, gout develops from abnormally high levels of uric acid in your blood that turn into painful crystals called tophi.
Uric acid (or urate) is a naturally-occuring byproduct in our body that comes from the breakdown of cells. It is also a byproduct of purines that are found in our food, which turn to uric acid when broken down by our digestive system. While our kidneys are meant to process uric acid and keep our blood levels regulated, having too much uric acid in our system for too long will lead to it crystallising in our joints, creating the painful condition known as gout.
Gout is considered to have a genetic component, meaning that if you have a family member with gout, you have a higher risk of developing it yourself. Specifically, the genetic characteristics are those related to your kidneys, your gut and your liver that help excrete uric acid in your urine. Certain genes mean that the rate at which urate is processed by your body slows, leading to high concentrates in the blood.
With this said, gout is often linked to diet, or a combination of both genetic factors and diet. Certain foods like organ meats, beer and other types of alcohol, seafood and beverages sweetened by high-fructose corn syrup contain higher levels of purines, and therefore will break down into uric acid within your body. When high-purine foods are consumed regularly, this is enough to raise the uric acid levels in the blood and cause gout. This is why historically, gout was known as the rich man’s disease, as wealthier men and women that consumed more red meats, seafood and alcohol had a higher prevalence of gout.
Other risk factors for gout include:
Similar to rheumatoid arthritis, gout typically presents in flares that come on suddenly and can last from several days to several weeks. Typical signs and symptoms include:
While it is fairly easy for our podiatrists to identify gout when we see a flare, the only way to confidently diagnose gout is with a blood test that measures uric acid levels in your blood, paired with identifying urate crystals in your joint fluid from a small sample.
While medical imaging is not indicated for a gout diagnosis, it may be valuable in the later stages of gout - or if you’ve had flares for several years without a formal diagnosis - to assess any damage to your bones or cartilage to help guide your treatment plan.
Medical Management
Effectively managing gout starts with an appointment with your GP to understand the medication options available to you. Several medicines
exist that can help ease a gout flare when it starts, as well as help prevent future flares by trying to lower the amount of uric acid
levels in your blood. These can look like NSAIDs, prednisone or low dose colchicine, depending on your individual circumstances. Allopurinol
may be given during an acute gout flare, though it may not be suitable for everyone.
Dietary Management
While getting relief from gout symptoms if possible is important, it is also important to take steps to naturally lower your uric acid levels instead of relying on medication to artificially (and temporarily) manage your symptoms. This means switching to a diet filled with low-purine foods, including plenty of eggs, nuts, legumes, fruits, whole grains, low-fat daily products and poultry. You can still eat seafood - you just need to switch to ones lower in purines such as salmon, crab and herring.
Podiatric Management
Your podiatrist can be very valuable in helping you manage the consequences of gout on your feet. This can look like:
| Monday | 7:40am - 6:00pm |
| Tuesday | 7:40am - 6:00pm |
| Wednesday | 7:40am - 6:00pm |
| Thursday |
7:40am - 6:00pm |
| Friday | CLOSED |
| Saturday | CLOSED |
| Sunday | CLOSED |
Ground Floor, 344 Queen Street,
Brisbane City QLD 4000
| Monday | 7:40am - 6:00pm |
| Tuesday | 7:40am - 6:00pm |
| Wednesday | 7:40am - 6:00pm |
| Thursday |
7:40am - 6:30pm |
| Friday | 7:40am - 5:00pm |
| Saturday | 7:40am - 4:30pm |
| Sunday | CLOSED |
Newmarket Village, 114/400 Newmarket Rd, Newmarket QLD 4051