Jump to section
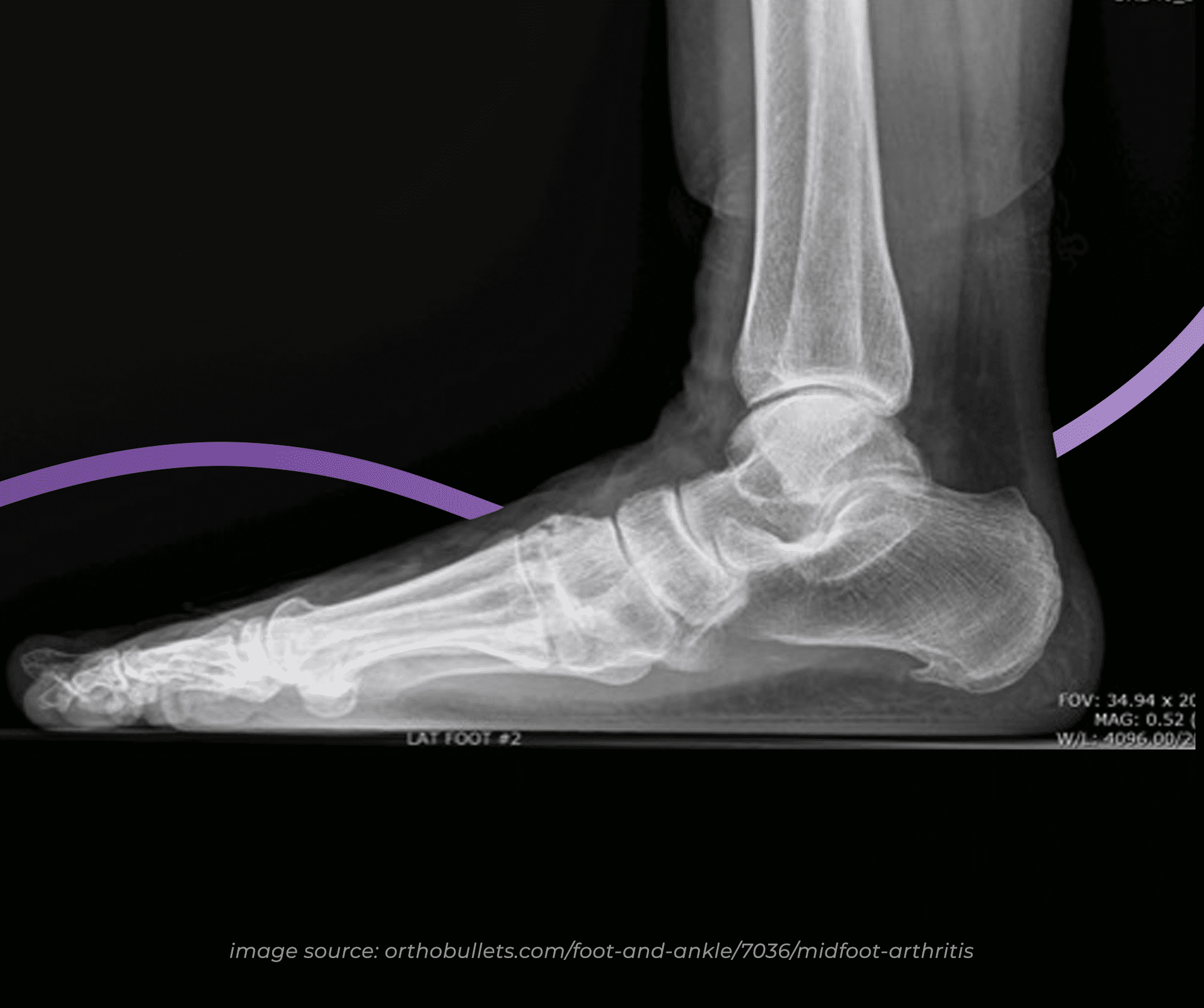
Generally speaking, osteoarthritis is best known as the wear-and-tear arthritis that occurs when the cartilage that covers and protects the
ends of the bones breaks down over time. This results in pain and swelling that can make the joints stiff and painful to move. In our
experience, arthritis that presents specifically in the midfoot is both underdiagnosed, and not managed to the best capacity by many. This
is why midfoot arthritis is an area of interest for our experienced Brisbane podiatrists.
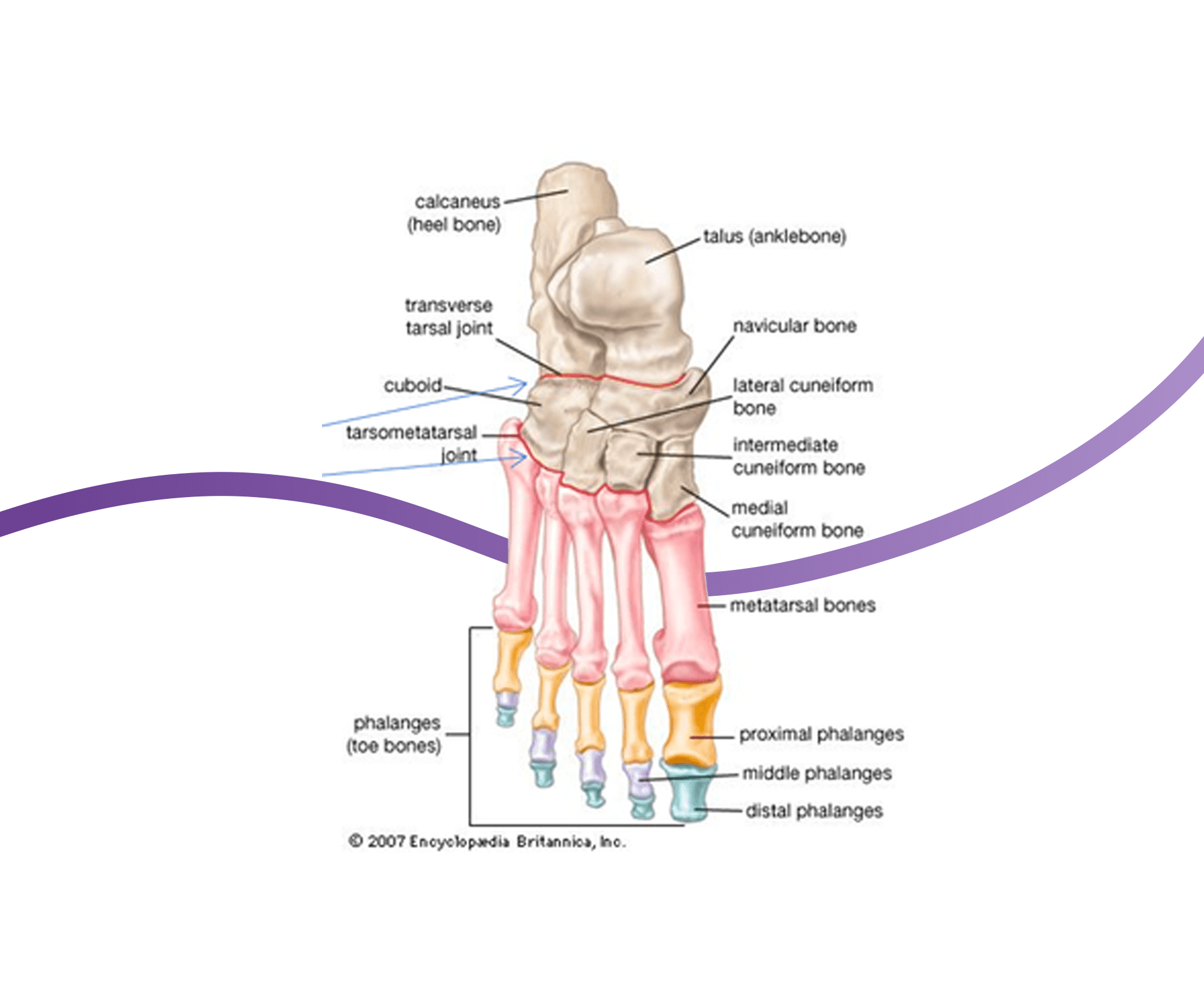
Midfoot arthritis is arthritis that occurs specifically in the mid-section of the foot, namely the tarso-metatarsal joints and naviculo-cuneiform joints. The midfoot is worthy of note as its own subsection of osteoarthritis due to the significant impact it has on the lives of our patients, and the careful, delicate and knowledgeable approach to treatment that it requires.
During each step, there is a great amount of force that crosses the midfoot as part of normal and necessary foot function, first when the foot ‘unlocks’, rolls down and adapts to the ground as we step down, and then as the foot prepares to toe off the ground and propel us forward as we walk or run. Longstanding compression at the midfoot (alongside other causes) can bring the midfoot joints painfully close together, rubbing against one another, and severely limiting the ability to participate in everyday activities.
Midfoot arthritis typically presents with pain beneath the foot that is exacerbated when walking or standing. Alongside this, many people experience:
Over time, when left unmanaged, midfoot osteoarthritis can result in a collapse of the midfoot, leading to a rigid flatfoot deformity with bony spurs being present. This can be very painful, alongside making wearing normal shoes difficult in terms of finding something that fits well and is comfortable.
While the most common cause of midfoot arthritis is gradual wear and tear, it has five different categories that the cause may fall under:
One important aspect of ‘wear and tear’ degenerative damage is the role our shoes can play. When we recommend good supportive shoes with a stiffer sole in the midfoot, we do so because our midfoot naturally does not (and should not) bend. Many shoes are designed in alignment with this, but some unsupportive footwear does allow for this unnatural bending, which can add more compressive forces on the midfoot, promoting degeneration.
Diagnosing midfoot arthritis includes taking a history and physical examination with your podiatrist, who will also work through ruling out the other potential causes of midfoot pain, and then using x-rays. Even if you are relatively confident that you have midfoot arthritis, x-rays can be extremely valuable in uncovering both the severity of your arthritis, and how many joints in the midfoot (and even beyond the midfoot) are affected. All of this information will be a helpful guide to your treatment.
The best way to manage midfoot arthritis will depend on your symptoms and the movement available at the midfoot. We always recommend non-surgical (conservative) treatment first, as many of our patients achieve significant pain relief and improvements in their day to day comfort without undergoing a painful procedure with a long recovery time.
Your treatment may include:
If your pain is causing disability that is not being relieved through non-surgical treatments, then fusion surgery may be required, where the damaged cartilage is removed and the joint is fixed in a permanent position, usually using a plate and screws or wires.
Surgery is not typically a first-line treatment for us, as our podiatrists achieve good success in significantly reducing pain and improving function with our conservative treatment options. Additionally, any surgery is not without its risk and potential complications. If our conservative methods fail to produce significant relief for you, however, then we can refer you to an orthopaedic surgeon to discuss the results that surgery could achieve given your unique circumstances.
Our feet are the foundation for the entire body, so it's important that they have enough strength to tolerate our activity levels. Use
these three exercises to help strengthen your feet.

Not everyone needs orthotics, but they can play an integral role in treating or relieving pain in several foot and lower limb conditions.

The heat and humidity of an Australian summer makes it a prime time for issues to arise, so our newest podiatrist Lucy has put together
seven helpful tips to keep your feet healthy and problem free throughout summer.
| Monday | 7:40am - 6:00pm |
| Tuesday | 7:40am - 6:00pm |
| Wednesday | 7:40am - 6:00pm |
| Thursday |
7:40am - 6:00pm |
| Friday | TEMP CLOSED |
| Saturday | CLOSED |
| Sunday | CLOSED |
Ground Floor, 344 Queen Street,
Brisbane City QLD 4000
| Monday | 7:40am - 6:00pm |
| Tuesday | 7:40am - 6:00pm |
| Wednesday | 7:40am - 6:00pm |
| Thursday |
7:40am - 6:30pm |
| Friday | 7:40am - 5:00pm |
| Saturday | 7:40am - 4:30pm |
| Sunday | CLOSED |
Newmarket Village, 114/400 Newmarket Rd, Newmarket QLD 4051