Jump to section
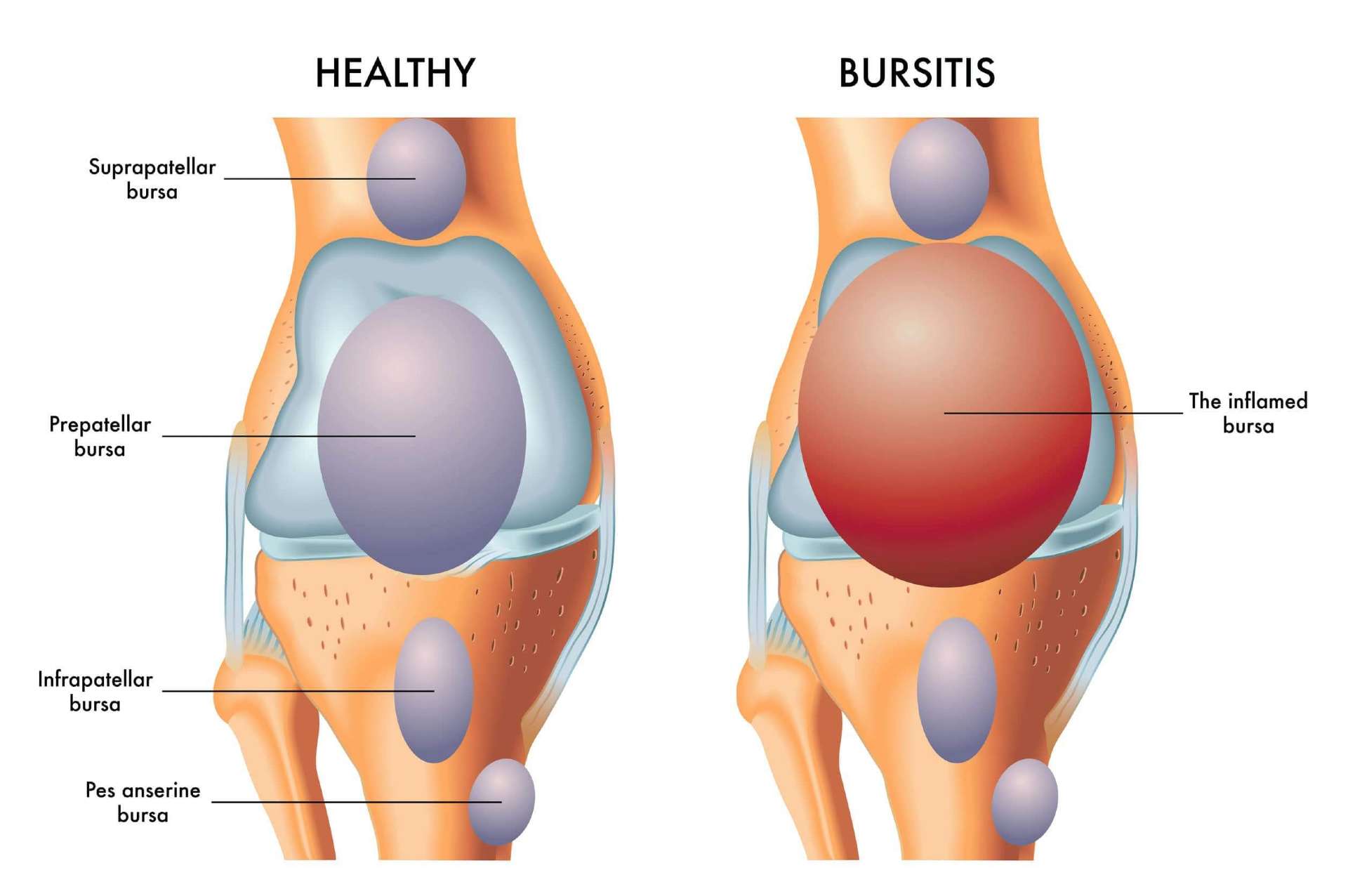
You can think of a bursa (or bursae for plural) as a small cushion that sits between a bone and a tendon, helping them move smoothly together as your body moves throughout your day. Getting a little more technical, bursae are fluid-filled, semi-compressible, sac-like structures that facilitate healthy, frictionless movement in our musculoskeletal system.
There are over 140 bursae in the body, and without them, our tendons, ligaments, tendons, and muscles would not be able to move smoothly with the bones when using the joint.
When bursae are exposed to higher levels of stress and/or irritation, they become inflamed, enlarged and painful. This condition is called bursitis.
The most common cause of bursitis is overuse and repetitive movements. A few examples of repeated movements that may cause
bursae to become irritated and damaged are gardening, painting, cleaning, running, cycling, golf and tennis.
Other causes of bursitis include:
Considering the potential causes of bursitis, there are certain factors that can increase your risk of developing the condition:
Bursitis commonly occurs around major joints like your hip, knee, ankle and heel. If you start to experience localised pain at these joints with or without swelling, then you may have bursitis.
Other bursitis symptoms associated with the condition may include:
Our podiatrists in Brisbane can see and treat all of the following areas where bursitis may occur:
The signs and symptoms of bursitis closely resemble those of tendonitis (inflammation of a tendon), so it's important that our podiatrists are able to correctly diagnose your condition.
To diagnose bursitis, we would first complete a physical assessment of the area and further specialised
bursitis assessments. Once pain is replicated, ultrasound imaging may be used to confirm the diagnosis of bursitis and to see if the
nerve has been impinged or damaged.
When treating bursitis, we will often suggest a personalised combination of the following treatments to allow you to achieve the fastest and most effective recovery.
Your bursitis is likely to improve in a few days or weeks if you rest and treat the affected area. Unfortunately, if you don't take action to treat the underlying cause, like by stretching and strengthening the muscles around the joint and modifying your daily activities or exercise, the problem is likely to continue to return.
While not all types of bursitis can be prevented, the following activities may help to reduce your risk:
Our feet are the foundation for the entire body, so it's important that they have enough strength to tolerate our activity levels. Use
these three exercises to help strengthen your feet.

Not everyone needs orthotics, but they can play an integral role in treating or relieving pain in several foot and lower limb conditions.

The heat and humidity of an Australian summer makes it a prime time for issues to arise, so our newest podiatrist Lucy has put together
seven helpful tips to keep your feet healthy and problem free throughout summer.
| Monday | 7:40am - 6:00pm |
| Tuesday | 7:40am - 6:00pm |
| Wednesday | 7:40am - 6:00pm |
| Thursday |
7:40am - 6:00pm |
| Friday | CLOSED |
| Saturday | CLOSED |
| Sunday | CLOSED |
Ground Floor, 344 Queen Street,
Brisbane City QLD 4000
| Monday | 7:40am - 6:00pm |
| Tuesday | 7:40am - 6:00pm |
| Wednesday | 7:40am - 6:00pm |
| Thursday |
7:40am - 6:30pm |
| Friday | 7:40am - 5:00pm |
| Saturday | 7:40am - 4:30pm |
| Sunday | CLOSED |
Newmarket Village, 114/400 Newmarket Rd, Newmarket QLD 4051